Cervical Cancer and HIV
One woman dies of cervical cancer every two minutes, and HIV-infected women are at fives times greater risk. Task-sharing could help.
Cervical cancer poses a serious and persistent threat to women’s lives, with one woman dying of cervical cancer every two minutes. Human immunodeficiency virus (HIV)-infected women are up to five times more at risk.
This presents a powerful opportunity for life-saving collaboration between two critical global health communities: communicable and non-communicable diseases (NCDs).
Combining the approach to tackling both HIV and cervical cancer holds major benefits. The most effective way to prevent cervical cancer is vaccinating adolescents against the human papillomavirus (HPV), and with the success of antiretroviral treatment, HIV interventions are an ideal opportunity to vaccinate. They also present a critical opportunity to raise awareness of the symptoms and risks of cervical cancer, and to conduct screenings.
The recent UNAIDs report, Knowledge Is Power, highlights the importance of scaling up HIV testing worldwide – especially at a time when new diagnoses can continue to climb, most recently reported by the World Health Organization (WHO) in the European Region.
To reach the millions who do not know their status, we need universal access to HIV testing services. HIV testing should be as widely available as pregnancy testing,’ said Michel Sidibé, former executive director of UNAIDS.
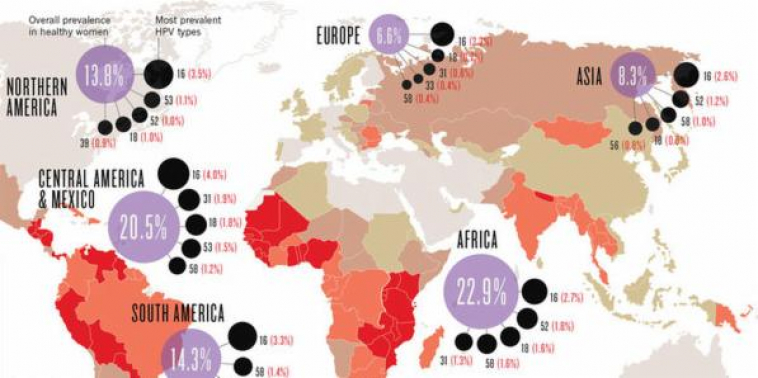
Cooperation is especially urgent in low-resource settings, where 9 out of 10 cervical cancer deaths occur and the majority of people diagnosed with HIV are living. 25.7 million out of 36.9 million people living with HIV are in the African region, where cervical cancer is also the leading cause of cancer death but HPV-research is unevenly funded. Task-sharing would therefore provide greater protection for millions of vulnerable people at risk of developing another life-threatening illness.
According to Professor Lynette Denny, past chair of FIGO’s Gynecologic Oncology Committee, and Chair of Obstetrics and Gynaecology at the University of Cape Town, South Africa:
“The ‘dual epidemics’ of HIV and cervical cancer and its precursors, are responsible for the premature deaths of thousands of women in the poorest countries of the world, mostly in the Global South. Lack of uptake or access to high quality preventative care is critical, but cannot be operationalised without the implementation of stronger and more reliable health systems that focus on the most important burden of disease, and the impact of the failure to allocate resources appropriately.”
In our recent Global Declaration on Cervical Cancer Elimination, FIGO underlined our commitment to collaborate on the global effort. National action must be accelerated, but equally the increased associated risk for those living with HIV must be acknowledged. Moving forward, any narrative surrounding the fight against cervical cancer must include an element of HIV prevention, treatment, counselling and care, and should ideally be part of an integrated healthcare package.
Both HIV and cervical cancer have a common theme: inequality of care. We need to work together to end the pain and anguish of women suffering from one, the other, and both. Task-sharing is a compassionate, dynamic approach that could have a long-term impact on two of the most pressing problems in sexual and reproductive health, and it cannot be overlooked.
Image courtesy of National Cancer Institute / World RePORT.