HPV testing in El Salvador
FIGO is committed to ensuring coordinated global action on the elimination of cervical cancer, uniting our network with the World Health Organization (WHO) and UNFPA.
We are proud of our member societies and colleagues driving change at national level, through their practice, advocacy - and crucially through their research, as a new study from El Salvador shows.
The cost‐effectiveness of implementing HPV testing for cervical cancer screening in El Salvador, published in the April issue of the International Journal of Gynecology and Obstetrics (IJGO), strengthens recommendations for effective and affordable cervical cancer screening and treatment strategies in low- and middle-income countries.
Said Dr. Miguel Antonio Guidos Serrano, President of ASOGOES (Asociación de Ginecología y Obstetricia de El Salvador):
“Cervical cancer elimination is a priority for us because it is a disease that can be prevented by extensive screening programmes, yet gynecologic cancers remain one of the most critical health issues affecting women in our country.”
ASOGOES has a strong voice on El Salvador’s National Cancer Committee, which advises the Ministry of Health on development of cervical cancer interventions. Lack of resources is an ongoing challenge, even as the Ministry and Social Security Institute (ISS) work to invest in expansion of early detection initiatives. Cost-efficiency studies are therefore particularly useful.
Explained Dr Guidos:
“International cooperation is very limited, since most organisations prioritise other diseases specific to women that produce a heavy burden of mortality, such as pregnancy care, access to modern contraception, HIV / AIDS and emerging diseases.
Our role as the national OBGYN society is to support cervical cancer elimination efforts through conferences, workshops, and seminars that strengthen health personnel knowledge. And as individual clinicians we are on the frontline of early detection of the disease, through routine check-ups we provide to our patients across the public and private health system.”
FIGO spoke to two of the IJGO clinical article authors, Associate Professor Miriam Cremer, President/Founder BHI and Dr Mauricio Maza, Executive Director at BHI, about their research.
Why does the epidemiology of cervical cancer in El Salvador make it particularly important to address the cost-effectiveness of prevention?
Cervical cancer is the leading cause of cancer death in El Salvador. As new technologies and management algorithms emerge for screening and prevention, it is important for those working in lower-resource settings to have an understanding of the impact of these new approaches. Where resources are limited, it is also important to understand which interventions will be the winning strategy from a cost effective point of view.
What did you find most interesting or surprising about the results of your study?
We confirmed that as we scaled the Cervical Cancer Prevention in El Salvador (CAPE) programme, the ‘screen and treat’ strategy remained a very cost-effective intervention compared to pap/HPV followed by colposcopy. This reassured us that it was the best intervention we could implement for El Salvador’s setting.
What have the responses of the women who have taken part in the CAPE project been like?
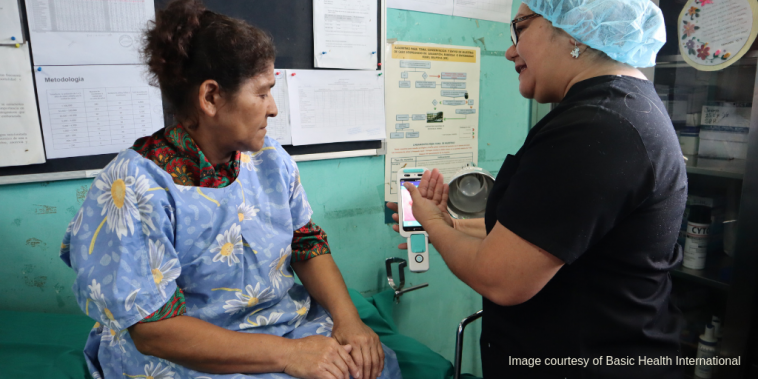
Patients (and providers) have been really pleased with the CAPE programme overall. We now have the capacity to use a low-cost test to screen for the underlying high-risk HPV types that cause cervical cancer. This is a vast improvement over current cytology programs, and it will save lives.
What have you found to be most rewarding about your work on the CAPE project?
Working in collaboration with the Ministry of Health has been very rewarding. Our group has the opportunity to make a difference in a public health setting.
El Salvador was the first country in the world to procure this low-cost HPV test for a national screening programme, and we believe it can serve as a model for other limited-resource settings that wants to implement HPV testing as a country-wide screening program.
How does your study fit with ongoing global efforts to eliminate cervical cancer?
It is a very exciting time in cervical cancer prevention. In May of 2018, World Health Organization (WHO) Director-General Dr. Tedros Adhanom Ghebreyesus announced a call to action for the global elimination of cervical cancer by 2030, declaring that cervical cancer is preventable and that the tools to eliminate it already exist.
Basic Health International (BHI) has been at the forefront of this initiative for almost 15 years. This study demonstrates the power of screen and treat interventions, and we are proud to be part of a global effort to end cervical cancer and help women continue to lead healthy lives.
Is there any advice you would like to share with other OBGYN practitioners around the world who are considering or planning to carry out similar cervical cancer prevention programs?
Get started! We have all the tools that we need to eliminate this preventable disease. We have so many technologies and so many alternatives of management for women who screen positive, and we must remember that we need to ensure proper follow up for all women at risk.