Preserving fertility before cancer treatment
Fertility after cancer is a concern for many women diagnosed during their reproductive years, but fertility preservation represents a real opportunity to improve their quality of life.
Oncology, the branch of medicine dealing with cancer, has offered millions of women and children the opportunity to fight and survive their diagnosis, but the surgical, chemo and radiotherapies employed can be harsh.
In many cases, due to the fast turnover of reproductive cells, cancer therapy can permanently, temporary or partially affect reproductive function.
Fertility preservation, a relatively new field of medicine, recognises that while improvement of the survival rate is essential, it must be accompanied by enhancing quality of life in the long-term.
Limiting the risk of infertility subsequent to cancer treatments is therefore essential.
This is why oncologists in conjunction with reproductive endocrinologists are increasingly discussing not only the impact of cancer treatments upon future fertility, but also the available methods for patients to maintain or safeguard future fertility, even as they continue therapies aimed to cure their cancer.
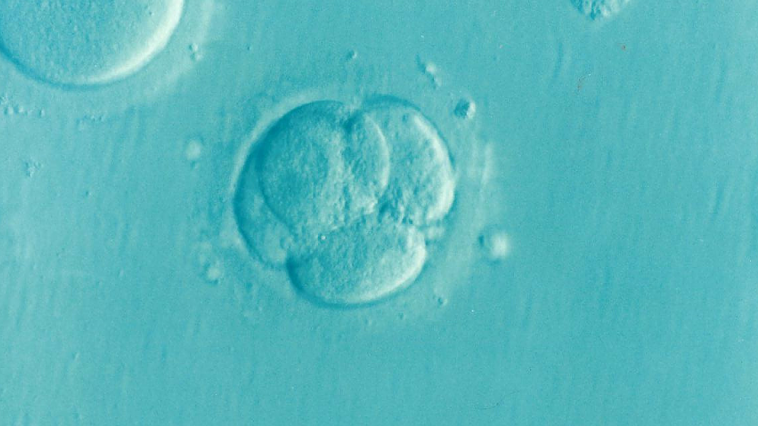
Previously, embryo freezing (cryopreservation) was the only effective and validated technique for preserving female fertility. Its main limitation is the nature of the embryo itself: binding the reproductive cells of two individuals together for later use raises concerns if one of the partners no longer exists.
Newer technologies have allowed women to preserve their fertility without the commitment and challenges of creating an embryo.
Egg freezing (oocyte vitrification) is now the gold standard of fertility preservation in women, and several thousand healthy children have born after this procedure. The birth rate depends on two factors: the number of mature cells (oocytes) retrieved, and the age of the patient at the time of the procedure. The younger the patient the more likely she has good oocytes and a better chance to conceive after thaw and usage of the frozen oocytes. The rates dramatically decrease after 40 years of age.
Numerous techniques have been developed for ovarian stimulation to adjust specifically to the particularities of the female population with cancer.
Another technique of fertility preservation, freezing of ovarian tissue rather than eggs, is still considered experimental in many countries – although the number of successful births with this method has increased in the last three years, now exceeding 100. This is the best option for girls before puberty, as well as patients who cannot undergo the ovarian stimulation necessary for mature egg retrieval due to lack of time, and should be considered a validated technique as studies to improve effectiveness and reduce risk are ongoing.
Fertility preservation represents a real opportunity to improve the quality of life of cancer survivors, and FIGO considers that all suitable oncology patients should be referred for a fertility preservation consultation as part of their routine cancer care, alongside counselling, a medical discussion of intervention, and consent.
Collaboration between the oncologic and reproductive teams treating a patient with cancer is essential, as a return to life-saving cancer treatment can typically be initiated within two weeks of commencing these fertility interventions.
Time has come for all doctors and patients to work together towards offering and receiving support, counselling, and the option of fertility preservation before cancer treatment when fertility can be compromised.